Why Do My Eyes Feel Dry All the Time? A Guide to Dry Eye Disease
If your eyes feel gritty, tired, or irritated by the end of the day — or even first thing in the morning — you are not alone. Dry eye disease is one of the most common conditions we see at our practice, and it is often misunderstood.
Many people assume dry eyes are simply the result of staring at screens too long or not sleeping enough. While those things can make symptoms worse, dry eye disease is a real, chronic condition with identifiable causes and it often goes undiagnosed for years.
What is dry eye disease?
Dry eye disease, also called dry eye syndrome or DED, is a condition in which the eyes either do not produce enough tears, or the tears do not function properly and evaporate too quickly to keep the eye surface properly lubricated.
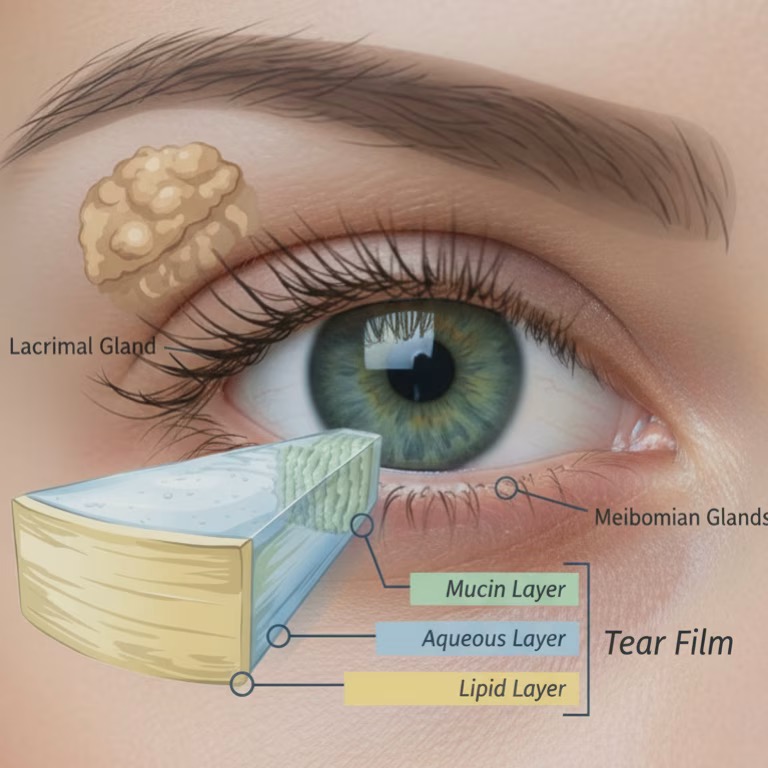
Your tear film is more complex than it might seem. It has two main phases: an outer lipid layer produced by the meibomian glands in your eyelids, and a deeper mucoaqueous layer, a single integrated phase in which water and mucin work together to keep tears stable and spread evenly across the eye. When either phase is disrupted, the entire tear film becomes unstable.
An unstable tear film cannot protect the surface of the eye the way it should. Over time, this leads to inflammation, discomfort, and sometimes damage to the front surface of the eye.
What does dry eye feel like?
Symptoms vary from person to person and can range from mildly bothersome to significantly disruptive. Some of the most common include:
- Dryness or grittiness — A feeling that something is in your eye, even when nothing is there.
- Burning or stinging — Especially noticeable in dry or windy environments, or with air conditioning.
- Watery eyes — A reflex response to irritation; the eye overproduces tears when the surface is disrupted.
- Blurry or fluctuating vision — Vision that clears temporarily when you blink, then blurs again shortly after.
- Eye fatigue — Eyes that feel tired, heavy, or strained, particularly with reading or screen use.
- Light sensitivity — Increased discomfort in bright light or with prolonged exposure to screens.
What causes dry eye disease?
Dry eye disease generally falls into two main categories, though many patients have a combination of both.
Aqueous deficient dry eye
In this type, the lacrimal glands do not produce enough of the watery component of the tear film. It is generally less common than evaporative dry eye and has a wide range of causes, including age-related lacrimal gland decline, certain medications, prior refractive surgery such as LASIK, and systemic conditions. Among systemic causes, autoimmune disorders, most notably Sjögren’s syndrome, are especially important to consider.
Evaporative dry eye
This is the most common type. Tears evaporate too quickly, often because the meibomian glands in the eyelids are not producing or delivering enough healthy oil to slow evaporation.
Meibomian gland dysfunction (MGD)
The meibomian glands are small oil-producing glands located along the edges of your eyelids. In many patients with dry eye, these glands become blocked or begin to produce oil of poorer quality. Without a healthy oil layer, tears can evaporate too quickly even if the eye is still making the watery component of tears.
Meibomian gland dysfunction is widely recognized as a leading contributor to evaporative dry eye disease and one of the most common drivers of dry-eye symptoms. It is also one of the conditions we evaluate closely during a dry eye examination at our practice.
Who is more likely to develop dry eye?
While dry eye disease can affect anyone, certain factors may increase the likelihood of developing it or worsening existing symptoms:
- Age: Dry eye becomes more common with age, and the risk continues to rise in older adults.
- Hormonal changes: Hormonal changes, especially around menopause, can increase dry-eye risk. Thyroid eye disease, especially when associated with Graves disease, can also contribute to dry-eye symptoms.
- Extended screen use: Reduced blink rate during screen time can make the tear film less stable and worsen dry-eye symptoms.
- Contact lens wear: Contact lenses can contribute to dryness and discomfort by affecting the tear film and ocular surface.
- Environmental factors: Dry climates, air conditioning, heating, wind, and smoke can all accelerate tear evaporation.
- Certain medications: Including antihistamines, antidepressants, blood pressure medications, and decongestants.
- Autoimmune conditions: Such as Sjögren’s syndrome, rheumatoid arthritis, and lupus.
- Prior eye surgery: Including LASIK, which can temporarily or persistently affect corneal nerves involved in tear production.
Is dry eye disease serious?
For many people, dry eye is a chronic condition that affects quality of life significantly, making it harder to read, drive, work at a computer, or wear contact lenses comfortably. In more persistent cases, chronic inflammation on the eye surface can contribute to damage to the corneal epithelium, which may affect comfort and vision if left untreated.
The good news is that dry eye disease is a manageable condition. A proper evaluation is the essential first step, because without identifying the main contributors to your dry eye, treatment is often less targeted and less effective.
When should you have your eyes evaluated?
We recommend scheduling a dry eye evaluation if you experience any of the following on a recurring basis:
- Persistent dryness, grittiness, or burning that does not resolve on its own
- Fluctuating vision that improves with blinking
- Eye discomfort that limits your ability to use screens, read, or drive
- Watery eyes that seem to have no clear cause
- Contact lens discomfort that was not present when you first began wearing lenses
- Over-the-counter eye drops that provide only brief or no relief
A comprehensive dry eye evaluation goes well beyond a standard eye exam. At RevitalEyes Optometry, we assess tear film quality and stability, evaluate the meibomian glands, and look for signs of inflammation on the eye surface, all of which inform a more targeted and effective treatment approach.
Ready to find out what’s causing your symptoms?
If you have been experiencing dry eye symptoms and would like a thorough evaluation, our team is here to help. We welcome new patients and same-day appointments may be available.